Living with occipital neuralgia is akin to fighting an invisible battle, one where the pain is as much internal as it is misunderstood by those around me. For years, I’ve navigated through life with a constant companion: a throbbing, piercing headache that seems to emanate from the base of my skull, wrapping its tendrils around my head and squeezing until I can find no relief. This journey has been one of frustration, discovery, and learning—a path that has led me to understand the complex condition known as occipital neuralgia.

Occipital neuralgia is more than just a headache; it’s a chronic pain condition that affects the occipital nerves, which run from the top of the spinal cord up through the scalp. The pain can be sharp, dull, or feel like an electric shock in the back of the head and neck. For those of us living with this condition, it’s not just about managing physical pain but also navigating the emotional and mental toll it takes.
This article is not just a recount of my struggles but a beacon for others like me, who may feel lost in their quest for answers and relief. It’s a deep dive into what occipital neuralgia is, the potential causes behind it, and the myriad ways to seek treatment and solace. My journey is unique, yet it reflects the shared experiences of many who live with this unseen battle of headaches and heartaches. Let’s explore together the shadows cast by occipital neuralgia and the paths that lead us toward light.

Understanding Occipital Neuralgia
For over five years now, since the fall of 2018, I’ve been living with a condition that, for a long time, felt like a puzzle I couldn’t solve. My journey began with unexplained headaches and neck pain, a relentless discomfort that made even the simplest tasks feel monumental. Bending forward became a trigger for intense pain, my neck seemed to be in a constant state of discomfort, and dizziness and a foggy feeling became my unwelcome companions. The sensation of pressure in my ears only added to the cacophony of symptoms, making me feel trapped within my own body.
What is Occipital Neuralgia?
Occipital neuralgia is a neurological condition characterized by chronic pain in the back of the head, neck, and behind the eyes. The pain is attributed to the occipital nerves, which can become inflamed or irritated, though the exact cause often remains elusive. Symptoms can mimic those of migraines or other types of headaches, making diagnosis a challenge. For me, the pain was not just a headache; it was a sharp, jabbing, electric shock-like sensation that made everyday life a struggle.
Symptoms That Differentiate It
The hallmark of occipital neuralgia is the pain’s location and nature. Unlike typical headaches, occipital neuralgia sufferers experience:
- Sharp, shooting pains that originate at the base of the skull and can radiate towards the scalp or down the neck.
- A persistent ache that feels like a tight band around the head.
- Sensitivity to light, making it difficult to be in brightly lit environments.
- Dizziness and a foggy sensation, as if one is not fully present in the moment.
Living with these symptoms has been a test of endurance. The pain is not just physical; it casts a shadow over your mental and emotional well-being, making you yearn for even a moment of relief.
The Challenge of Living with an Invisible Condition
One of the most difficult aspects of living with occipital neuralgia is its invisibility. To the outside world, you look fine, making it hard for others to understand the severity of your pain. This invisibility can lead to a sense of isolation, as if you’re battling a ghost that only you can feel.
Despite undergoing an MRI and trying physical therapy, relief has remained elusive. The journey has been a cycle of hope and disappointment, with each failed attempt at treatment feeling like a step back into the shadows. Yet, it’s a journey I continue to navigate, armed with the hope that understanding and relief are on the horizon.

The Why Behind the Pain: Unraveling the Causes of Occipital Neuralgia
In my relentless search for answers, I’ve delved into the myriad causes of occipital neuralgia, seeking to understand why this condition chose me. The reasons behind occipital neuralgia are as varied as they are complex, involving a combination of physical stress, potential nerve damage, or even underlying health issues that can exacerbate the condition.
Possible Causes and Triggers
Occipital neuralgia can stem from a variety of sources, including:
- Muscle tension and stress: Prolonged tension in the neck muscles can compress the occipital nerves, leading to inflammation and pain.
- Trauma or injury: A direct blow to the head, neck injuries, or even whiplash can trigger occipital neuralgia.
- Nerve compression: Conditions like cervical disc disease or arthritis can compress the occipital nerves, causing the characteristic pain of occipital neuralgia.
In my case, the cause wasn’t immediately clear, which only added to my frustration. The symptoms—dizziness, neck pain, and that ever-present foggy feeling—suggested a tangled web of potential triggers, making it challenging to pinpoint a single source.
The Complexity of Diagnosis
Diagnosing occipital neuralgia is a journey fraught with challenges. The condition’s symptoms overlap with those of other headaches, such as migraines or tension headaches, leading to misdiagnosis or delayed treatment. For me, an MRI and physical therapy sessions were steps on this journey, yet they offered no definitive answers, only more questions.
The bending forward that brings about such intense discomfort, the constant neck pain, the dizziness, and the pressure I feel in my ears all point towards a complex condition that requires a nuanced approach to treatment. It’s a reminder of the intricate relationship between our bodies’ physical structures and our nervous system.
Exploring Related Conditions
As I navigated through this maze of symptoms and potential causes, I discovered that occipital neuralgia often doesn’t exist in isolation. Conditions like neck arthritis can play a significant role in its development, contributing to the nerve compression that triggers occipital neuralgia. For those interested in exploring the connection between neck pain, dizziness, and underlying conditions like neck arthritis, I found Neck Arthritis Unveiled: More Than Just Pain to be an insightful resource. It sheds light on the hidden symptoms and the broader impact of neck conditions, offering valuable information for anyone navigating similar health challenges.
Living with occipital neuralgia is a daily exercise in patience and perseverance. Each day brings its own set of challenges, but it also offers new opportunities to learn and adapt. In understanding the “why” behind the pain, I’ve found a sense of empowerment—a knowledge that, while the battle may be unseen, it is not unwinnable.

Triggers That Intensify Occipital Neuralgia Symptoms
Living with occipital neuralgia has been akin to navigating a ship through a storm, where certain triggers can suddenly intensify the tempest of symptoms, making the journey even more tumultuous. Over these five years, I’ve become acutely aware of the factors that exacerbate my condition, learning to either avoid them or brace myself for the impact.
Physical Stress and Poor Posture
One of the most significant triggers I’ve encountered is physical stress, especially related to poor posture. Hours spent hunched over a computer or looking down at a smartphone can tighten the neck muscles, compressing the occipital nerves and setting off a cascade of pain. It’s a modern-day malady that requires constant vigilance to mitigate.
Environmental Factors
Bright lights and loud noises aren’t just sensory overload; they’re also triggers that can amplify my symptoms. Environments with harsh lighting or significant auditory stimuli can quickly lead from discomfort to unbearable pain, a reminder of the condition’s sensitivity to external inputs.
Weather Changes
Interestingly, shifts in weather patterns, especially abrupt changes in barometric pressure, seem to have a direct line to my occipital neuralgia symptoms. Storm fronts, drastic temperature drops, or even the approach of rain can herald an increase in headache intensity, a phenomenon that’s both fascinating and frustrating.
Physical Activity
While exercise is generally beneficial for health, certain types of physical activity can worsen occipital neuralgia symptoms. High-impact exercises, abrupt movements, or even just bending forward can provoke sharp increases in pain, limiting my ability to engage in activities I once enjoyed without a second thought.
Stress and Fatigue
The twin specters of stress and fatigue are ever-present in modern life, and they play a significant role in exacerbating occipital neuralgia. Emotional stress can lead to physical tension, particularly in the neck and shoulders, while fatigue can lower my threshold for pain, making the symptoms feel more intense.
Understanding and identifying these triggers has been a crucial part of managing my occipital neuralgia. It’s a delicate balance, one that requires constant attention and adaptation. While avoiding these triggers doesn’t cure the condition, it does offer a semblance of control, a way to navigate the storm with a bit more confidence.
Does Occipital Neuralgia Cause Pain Beyond the Head?
In my journey with occipital neuralgia, one of the most perplexing aspects has been the seemingly boundless reach of its symptoms. Beyond the characteristic headaches and neck pain, I’ve encountered moments where the discomfort extends far beyond, sending shocks of nerve pain down my arm and even making my fingers hurt. This extension of pain challenges the misconception that occipital neuralgia’s impact is confined to the head and neck.
The Radiating Nature of Nerve Pain
Occipital neuralgia, at its core, is a nerve-related condition. The occipital nerves, responsible for much of the pain associated with this condition, have a complex network. When these nerves are compressed or irritated, the pain doesn’t always stay localized; it can radiate. For me, this radiating pain manifests as sharp, shooting sensations that extend down the back of my neck, into my shoulders, down my arm, and even into my fingers.
Understanding the Connection
The phenomenon of pain radiating to the arms and fingers can be attributed to the interconnected nature of our body’s nervous system. The occipital nerves, while primarily located at the base of the skull, are part of a larger network that interacts with other nerves in the neck and spine. When occipital neuralgia triggers nerve pain, it can inadvertently affect these connected pathways, leading to sensations in areas seemingly unrelated to the condition’s typical domain.
Personal Experience with Radiating Pain
There have been days when the pain seemed to cascade down my body like a domino effect, from the back of my head, through my neck, down my arm, and to my fingertips. These episodes are not only painful but also bewildering, making me question how a headache can have such far-reaching effects. The pain in my fingers, in particular, serves as a stark reminder of the pervasive nature of nerve pain and the intricate web of connections within our bodies.
Coping with Extended Symptoms
Managing these extended symptoms involves a multi-faceted approach. From physical therapy designed to relieve nerve compression to relaxation techniques aimed at reducing overall stress and tension, I’ve explored various strategies to mitigate the impact of this radiating pain. It’s a process of trial and error, learning to listen to my body and respond with kindness.
Occipital neuralgia’s ability to send nerve pain down the arm and make fingers hurt adds another layer of complexity to an already challenging condition. It underscores the importance of a comprehensive treatment plan that addresses not just the primary pain points but also the extended areas affected by nerve irritation. Living with this condition is a continual learning experience, one that teaches resilience in the face of pain and the interconnectedness of our bodies.

Can Occipital Neuralgia Lead to Dizziness, Nausea, or Lightheadedness?
In grappling with occipital neuralgia, I’ve been confronted with a spectrum of symptoms that extend beyond mere pain. Among the most disorienting and debilitating are dizziness, nausea, and a pervasive sense of lightheadedness. These symptoms weave a complex tapestry of discomfort, further complicating the daily battle with this condition.
The Link Between Occipital Neuralgia and Dizziness
Dizziness has been a frequent and unwelcome companion on my journey with occipital neuralgia. The sensation isn’t just about feeling unsteady; it’s an intense vertigo that can make even the most familiar environments seem alien and difficult to navigate. This symptom can be attributed to the close relationship between the occipital nerves and the body’s balance mechanisms. When these nerves are inflamed or irritated, it can disrupt the delicate balance maintained by the inner ear and the brain, leading to episodes of dizziness.
Nausea and Lightheadedness: Adding Insult to Injury
Nausea and lightheadedness often accompany dizziness, forming a trio of symptoms that can incapacitate even the strongest among us. The experience of nausea, in particular, adds a layer of physical discomfort that compounds the challenge of managing occipital neuralgia. For me, these symptoms are not just side effects; they are significant obstacles that impact every aspect of life, from work to personal relationships.
Understanding the Impact
The presence of dizziness, nausea, and lightheadedness in occipital neuralgia sufferers can be perplexing. It’s a reminder that the condition’s effects are not limited to pain but can also influence the body’s fundamental systems, such as balance and digestion. These symptoms can be triggered by the same factors that exacerbate the primary pain—stress, poor posture, and physical strain—further highlighting the interconnectedness of the body’s responses to occipital neuralgia.
Coping Strategies
Dealing with these symptoms requires a holistic approach to treatment and management. Techniques that promote relaxation and stress relief, such as meditation and gentle yoga, have been beneficial in reducing the frequency and intensity of dizziness and nausea. Additionally, maintaining a regular sleep schedule and staying hydrated have been crucial in managing lightheadedness, providing a foundation for stability amidst the chaos of occipital neuralgia.
Occipital neuralgia’s capacity to induce dizziness, nausea, and lightheadedness adds a challenging dimension to its management. These symptoms serve as stark reminders of the condition’s complexity and its profound impact on the sufferer’s quality of life. Navigating through these challenges requires patience, resilience, and a comprehensive approach to care that addresses both the physical and emotional aspects of the condition.
Does Occipital Neuralgia Affect Your Eyes?
Throughout my ongoing battle with occipital neuralgia, I’ve encountered a symptom that initially seemed unrelated: eye discomfort. Burning sensations, itchiness, and episodes of blurry vision have all manifested, adding layers of complexity to an already bewildering condition. These eye-related symptoms have led me to question, how can a nerve condition primarily known for causing headaches and neck pain also impact my eyes?
The Connection Between Occipital Neuralgia and Eye Symptoms
The link between occipital neuralgia and eye discomfort lies in the intricate network of nerves and their connections. The occipital nerves, while primarily located at the back of the head, are part of a complex system that can influence sensations in other areas, including the eyes. When these nerves are irritated or inflamed, it can trigger a cascade of reactions, leading to symptoms like burning eyes, itchiness, and blurred vision.
Burning and Itchy Eyes: A Nerve-Induced Discomfort
The sensation of burning or itchy eyes has been particularly perplexing and uncomfortable. This symptom can be so sudden and intense that it feels as though the eyes are being exposed to an irritant, yet there’s nothing visibly causing the discomfort. It’s a stark reminder of the power of nerve signals and how disturbances in one part of the nervous system can manifest in seemingly unrelated areas.
Blurry Vision: Navigating a World Out of Focus
Episodes of blurry vision have been among the most disconcerting symptoms associated with my occipital neuralgia. This visual disturbance can occur without warning, transforming the world into a blur and complicating tasks that require sharp visual focus. The mechanism behind this symptom is less about direct nerve irritation and more about the secondary effects of occipital neuralgia, such as muscle tension and stress, which can strain the eyes and lead to temporary vision changes.
Addressing Eye-Related Symptoms
Managing these eye-related symptoms has required a proactive and multifaceted approach. Ensuring regular eye rests, especially during prolonged periods of screen time, has been crucial. Additionally, using lubricating eye drops helps alleviate burning and itching sensations, while practicing stress-reduction techniques can mitigate the underlying triggers of these symptoms.
The impact of occipital neuralgia on the eyes is a testament to the condition’s complexity and the interconnectedness of the body’s systems. Eye discomfort, including burning sensations, itchiness, and blurry vision, underscores the wide-ranging effects of nerve irritation and inflammation. Coping with these symptoms involves not just addressing the eye discomfort directly but also tackling the broader challenges posed by occipital neuralgia.

Can Occipital Neuralgia Lead to Weakness, Tiredness, or Fatigue?
In my personal experience, occipital neuralgia has been more than just a source of pain; it has significantly impacted my overall energy levels, leading to feelings of weakness, tiredness, and fatigue. These symptoms, while perhaps less discussed, are equally debilitating, affecting my daily life and overall well-being.
Understanding the Impact on Energy Levels
The relentless nature of occipital neuralgia pain can be exhausting. Pain, especially when chronic, demands a continuous expenditure of energy from the body to cope with the discomfort and stress it causes. This constant battle can deplete energy reserves, leading to a state of fatigue that affects both physical and mental capacities.
Weakness and Tiredness as Secondary Symptoms
Feeling weak or experiencing generalized tiredness are symptoms that can arise as the body’s response to the ongoing stress of managing chronic pain. The effort to maintain normalcy in the face of persistent discomfort can be draining, leaving one feeling physically weak and perpetually tired. For me, these feelings of weakness and tiredness are not just about lacking physical strength or needing sleep; they represent a deeper level of fatigue that rests and sleep alone cannot fully alleviate.
The Cycle of Pain and Fatigue
Fatigue can exacerbate the experience of pain, creating a vicious cycle where pain leads to fatigue, which in turn can make the pain feel more intense. This cycle can be challenging to break and requires a multifaceted approach to manage effectively. In my journey, finding balance involves not only addressing the pain through medical treatments but also adopting lifestyle changes aimed at boosting energy levels and improving overall health.
Strategies for Managing Fatigue
Managing the fatigue associated with occipital neuralgia has been a crucial component of my overall treatment plan. This includes:
- Prioritizing good sleep hygiene to ensure restorative rest.
- Engaging in regular, gentle exercise as tolerated, which can help improve energy levels over time.
- Practicing stress-reduction techniques such as meditation or yoga to help the body relax and recover.
- Consulting with healthcare professionals to optimize pain management strategies, reducing the body’s stress response to pain.
Occipital neuralgia’s capacity to induce feelings of weakness, tiredness, and fatigue underscores the condition’s profound impact on one’s quality of life. Recognizing and addressing these symptoms is essential for anyone navigating the complexities of this condition. By adopting a comprehensive approach to management, it’s possible to mitigate some of the fatigue associated with occipital neuralgia, paving the way for improved energy levels and a better overall sense of well-being.
The Indirect Effects of Chronic Pain on the Body
Heart Palpitations
Heart palpitations, a sensation where the heart feels like it’s pounding, fluttering, or beating irregularly, can be a stress response. Chronic pain is a significant source of stress for the body, activating the “fight or flight” response which, in turn, can affect heart rate. For me, during particularly intense episodes of pain, I’ve noticed an increase in heart palpitations, highlighting the body’s interconnected response to stress and discomfort.
Stomach Issues
Similarly, stomach issues, including nausea, indigestion, or abdominal discomfort, can manifest as part of the body’s reaction to ongoing pain and stress. The gastrointestinal system is especially sensitive to stress, and chronic conditions like occipital neuralgia can trigger or exacerbate stomach problems. Personally, periods of heightened pain have often been accompanied by gastrointestinal discomfort, a reminder of the stress-pain connection.
Managing Stress-Related Symptoms
Recognizing that heart palpitations and stomach issues can arise as indirect effects of the stress and discomfort caused by occipital neuralgia, adopting stress management and relaxation techniques has been pivotal in my care regimen. Techniques such as deep breathing exercises, mindfulness meditation, and gentle physical activities like walking or yoga have helped in moderating the body’s stress response, potentially reducing the incidence of these stress-related symptoms.
The Importance of Holistic Care
The experience of heart palpitations and stomach issues alongside occipital neuralgia underscores the need for a holistic approach to managing chronic pain conditions. It’s crucial to not only address the pain itself but also the broader impacts on physical and emotional health. Consulting with healthcare professionals across different specialties can ensure that the management plan encompasses all aspects of well-being, including cardiovascular and gastrointestinal health.
Mapping the Pain: Understanding Occipital Neuralgia’s Reach
Occipital neuralgia, with its defining characteristic of nerve pain, casts a wide net in terms of the areas it affects. Through my own experiences, I’ve come to understand that while the epicenter of discomfort lies at the back of the head and neck, the pain doesn’t confine itself to these regions alone. The nature of this condition means that its impact can be felt in various locations, painting a complex picture of discomfort that can shift and change.
Primary Pain Locations
- Back of the Head: The hallmark of occipital neuralgia is the intense, sharp pain that originates at the base of the skull, where the occipital nerves exit the spine. This pain can be piercing and is often described as electric-shock-like.
- Scalp: The pain frequently radiates upwards, affecting the scalp. It can make the hair and skin feel incredibly sensitive, to the point where even a gentle touch or brush of hair can feel excruciating.
- Behind the Eyes: Although less intuitive, the pain from occipital neuralgia can radiate to the area behind the eyes. This can lead to a deep, aching sensation that exacerbates the discomfort of the headache.
Secondary Pain Locations
- Neck and Shoulders: The muscles in the neck and shoulders can become tense and sore as a response to the constant pain at the back of the head. This muscle tension can further aggravate the condition, creating a vicious cycle of pain.
- Upper Back: For some, the discomfort extends down into the upper back. Muscle tension and nerve irritation can contribute to a broader area of discomfort, emphasizing the interconnected nature of our body’s pain response.
- Ears: In some cases, occipital neuralgia can cause pain or sensitivity around the ears. While not as common, it’s a testament to the complex network of nerves and how pain signals can travel.
Navigating the Pain Map
Living with occipital neuralgia means becoming intimately familiar with these pain locations, learning to anticipate and manage discomfort in these areas. It requires a strategy that’s both reactive, to manage pain when it arises, and proactive, to prevent the escalation of symptoms.

Differential Diagnosis and the Quest for Answers
Occipital neuralgia, with its elusive nature and wide-ranging symptoms, often finds itself entangled in a complex web of differential diagnoses. Over the years, my quest for relief has led me down various paths, exploring conditions that mimic occipital neuralgia but require distinctly different treatments. This journey through the medical maze has been frustrating, leaving me to wonder why a definitive diagnosis remains just out of reach.
Common Conditions Mistaken for Occipital Neuralgia
- Migraines and Tension Headaches: The most frequent contenders, migraines and tension headaches, share several symptoms with occipital neuralgia, such as head pain and sensitivity to light. However, migraines often come with nausea and are typically one-sided, while tension headaches feature a band-like pressure around the head, lacking the sharp, shooting pain characteristic of occipital neuralgia.
- Cervicogenic Headaches: Originating from issues in the cervical spine, cervicogenic headaches can cause pain in the back of the head and neck, similar to occipital neuralgia. The key difference lies in the source of the pain, which for cervicogenic headaches, is the neck’s structural problems.
- Trigeminal Neuralgia: Another neuralgia, affecting the trigeminal nerve in the face, can sometimes be confused with occipital neuralgia due to the intense, shock-like pain it produces. However, trigeminal neuralgia primarily affects the face, not the back of the head or neck.
The Diagnostic Odyssey
Diagnosing occipital neuralgia is a process of elimination, requiring careful assessment to distinguish it from other conditions. The journey typically involves:
- Medical History and Physical Examination: A detailed discussion of symptoms and a physical exam focusing on the head, neck, and shoulders.
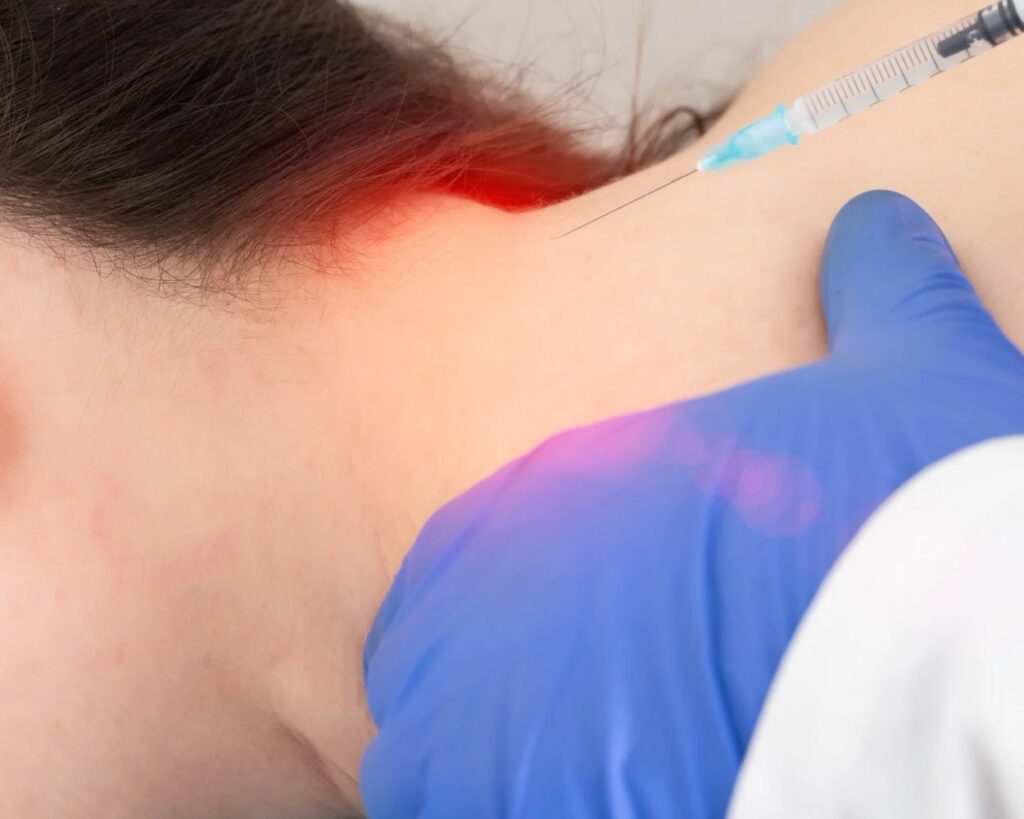
- Nerve Block Test: A diagnostic nerve block, where a local anesthetic is injected into the occipital region, can provide temporary relief. Significant pain reduction following the injection often points toward occipital neuralgia.
- Imaging Tests: While not definitive for occipital neuralgia, MRI or CT scans can help rule out other causes of headaches, such as tumors or structural issues.
The Elusive Diagnosis
The question of why a diagnosis remains elusive, despite years of investigation, reflects the complexity of the human nervous system and the subtleties of neuralgia conditions. Many healthcare providers are more familiar with common headache disorders like migraines, potentially overlooking less common conditions like occipital neuralgia. Additionally, the variability of symptoms and the lack of a single, definitive test for occipital neuralgia complicate the diagnostic process.
Finding Resolution
For those of us on this journey, the path to managing occipital neuralgia begins with a correct diagnosis, which itself starts with awareness and advocacy. Being informed about the condition, communicating effectively with healthcare providers, and seeking specialists familiar with neuralgias can make a significant difference.
In terms of treatment, options vary from nerve blocks and physical therapy to medications and, in some cases, surgery to decompress the affected nerves. The goal is to manage pain and improve quality of life, a process that often requires patience, persistence, and a tailored approach to care.
My journey with occipital neuralgia highlights the challenges and complexities of navigating the healthcare system in search of answers. It underscores the importance of determination, self-advocacy, and the hope that with the right diagnosis, effective management is within reach.
As an Amazon Associate we earn from qualifying purchases through some links in our articles.




